keratoplasty
What you will read...
What is keratoplasty?
The cornea is the clear front layer of the eye located just in front of the colored part (iris). It is completely transparent, allowing light to enter the eye, and also refracts or bends the light to focus images of objects, both near and far, onto the retina. Corneal transplant surgery, also known as keratoplasty, is a procedure in which a cloudy or damaged cornea is replaced with a clear cornea.
How does a defective cornea affect vision?
If the cornea of our eye becomes inflamed due to tissue swelling or becomes cloudy and loses its transparency, it is no longer smooth and polished. Corneal cloudiness, corneal swelling, or irregular corneal shape scatter light in different directions, creating an irregular image and causing blurred vision. For good vision, a smooth and transparent cornea is always necessary.
Corneal transplantation is a restorative treatment for which conditions?
- Keratoconus
- Corneal edema after eye surgeries like cataract surgery.
- Corneal opacities resulting from infections, especially ocular herpes
- Inherited corneal diseases like Fuchs' dystrophy
- Inherited corneal opacities like granular and macular dystrophy
- Corneal opacities following an injury or post-corneal injury
- Rejection of graft (in an eye that has been previously grafted)
The stages of corneal transplant before surgery
When a cornea specialist surgeon determines that your eye requires a transplant, they request a cornea for you from an eye bank. Before delivering the cornea, the eye bank conducts examinations to ensure it is free from infectious diseases such as hepatitis, HIV, etc., and checks for transparency. Your eye doctor will advise you on anesthesia and request necessary tests. If you are taking any specific medications, be sure to inform your doctor.
During the surgical procedure
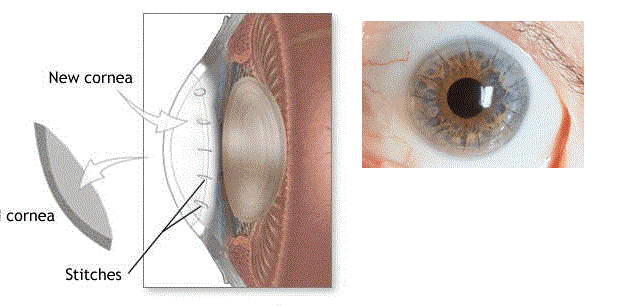
During eye surgery, your eye is held open using a tool called a speculum. The eye is carefully washed, and a cornea specialist examines it with a microscope, measuring your defective cornea and the donor cornea. The defective cornea is precisely removed from the eye, and additional procedures such as cataract removal may be performed if needed. Then, the healthy and transparent donor cornea is stitched in place. At the end of the procedure, a protective shield is placed over your eye.
If you experience the following symptoms, contact a doctor:
- Reduced vision compared to previous days.
- Eye pain and its surrounding area that does not resolve with prescribed pain relievers.
- Increased redness, swelling, and eye discharge.
- Sudden onset of pain above the eye "eyebrow area" and constant headache.
- Seeing colored halos around lights.
- Feeling fear and discomfort from light (photophobia).
- Feeling a foreign body sensation in the eye (which may be due to loosening or opening of sutures, and if sutures are not removed, the risk of graft rejection increases).
What is the Cornea Bank?
Prior to the 1970s, there was no suitable environment for preserving corneas and eyes, which is why corneal transplants were performed several hours after the donor’s death. From the early 1970s onwards, a suitable environment for preserving corneas and eyes became available on the market, which could keep the cornea healthy for several days to weeks. This made it possible to transport corneas to distant areas.
In eye banks, there are specific criteria for the usability of a cornea from a deceased person. If the individual had certain diseases, the cornea may not be suitable for transplantation.
Due to the spread of infectious diseases such as hepatitis and AIDS, laboratory tests are conducted before corneal transplantation. If these tests are negative, the corneal tissue is sent to transplantation centers. Corneas from individuals aged 1 to 70 years are generally considered suitable for transplantation, although the quality of the cornea may decrease with age.
Preoperative Recommendations
- After deciding to undergo the surgery and obtaining the physician's approval, you will be scheduled for a corneal transplant. The cost of the eye surgery is paid to the Bank of the Eye of the Islamic Republic of Iran. This fee is used for the preparation and testing of the donor cornea, including tests for diseases like AIDS, hepatitis, and others. The cornea itself is donated and provided free of charge.
- The bank receipt, along with the completed transplant form by the treating physician, is submitted to the Eye Bank.
- If you plan to use health insurance, it's better to visit the relevant insurance authority with the referral letter from the treating physician the day before the surgery and obtain the referral letter for the clinic where the operation will take place.
- If the treating physician needs to know, you should have blood and urine tests done at a nearby clinic or hospital one or two days before the surgery and bring the results to the clinic on the day of the operation.
- The day before the surgery, take a shower, and it's better if gentlemen shave their faces.
- On the day of the surgery, women should avoid wearing makeup, especially eye makeup.
- Be sure to take all the medications you have been prescribed for other conditions such as diabetes, high blood pressure, heart problems, etc., on the day of the surgery.
- If your surgery is performed under general anesthesia, do not eat breakfast. If it's done under local anesthesia, you may have breakfast with the doctor's approval.
- On the day of the surgery, you will visit the clinic for admission one hour before the operation.
- After entering the operating room, you will put on special attire. If there is a need for simultaneous cataract surgery, a nurse will administer dilating eye drops into your eyes several times.
- About half an hour later, you will go to the operating room with a nurse.
- After lying on the operating table, you will either be anesthetized, depending on your overall condition and the recommendation of the treating physician. You will not feel any pain during the procedure.
Postoperative recommendations
- Using eye makeup and products around the eyes should be avoided on the day of surgery.
- Eye wash and bathing.
- Exercising and heavy physical activities, as well as lifting heavy objects.
- Rubbing and touching your eyes.
- Coughing and sneezing.
- Sudden change in head position.
- Bending the head down to below the waist and prostrating. Do not go into prostration during prayer for 3 to 4 weeks, instead, place your forehead on the ground.
- Sleeping on your stomach or the side that has been operated on.
- Washing your hair and face with shampoo is not a problem after the first week following the surgery, provided your doctor approves.
- It is prohibited to drive due to insufficient vision.
- After you are allowed to shower, avoid getting water inside your eyes for 3 to 4 weeks. Also, refrain from rubbing your eyes during bathing.
Prescribing glasses after a corneal transplant
In many cases of transplantation, after the surgery, eyeglasses or contact lenses will be prescribed to correct refractive errors (nearsightedness, farsightedness, astigmatism), but nowadays, it is possible to use LASIK as an alternative method.
